Public Health
A Behavioural Insights Approach to Clinical Trial Enrollment
2023
PARTNERS
Leukemia & Lymphoma Society (LLS)
Share
The Behaviouralist worked with the Leukemia & Lymphoma Society (LLS) to investigate the barriers to clinical trial enrollment of blood cancer patients within the Veterans Health Administration (VHA) system in the US.
Clinical trials are essential for the development of new treatments and can also offer superior care to patients who are enrolled; however, despite these benefits, few patients enrol in clinical trials, a dearth that is particularly prevalent within the Veterans Health Administration (VHA).The VHA is the largest integrated health service provider in the United States, providing care to over 450,000 veterans and diagnosing 43,000 new cases annually. Though many of these patients could benefit from clinical trials, few are referred to trials or choose to enrol.
To understand the barriers to clinical trial referral among VHA providers, The Behaviouralist employed a mixed-methods approach, which included completing a comprehensive literature review, developing and fielding a survey and conducting a series of semi-structured interviews to capture providers' attitudes, beliefs, and experiences regarding oncology clinical trial referral and enrolment. The summation of these exercises were captured in a behavioural journey map, a visual representation of the decision making process that VHA providers move through when considering referring a patient to a clinical trial.
We surveyed practitioners to identify the determinants and drivers of clinical trial referrals.
The survey, developed in collaboration with the LLS team, captured providers’ experience with clinical trials, how they recruit and communicate with patients, and strategies to enhance clinical trial enrollment. The survey also collected socio-demographic information about the providers.
The survey was distributed via email to 84 VHA providers. A total of 34 complete responses were collected and included in the analysis.
Several key insights were gleaned from the survey data:
- The most common first action taken when enrolling patients to clinical trials was identifying appropriate trials for their patients, while the last action taken was facilitating referrals for specific trials.
- The most frequently experienced concern was that there are no are no appropriate trials within the VA, followed by that the patient is unlikely to be eligible for any trial.
- Lack of transportation was the most frequently experienced patient concern. The second most frequent concern was lack of time.
- Ensuring high quality care for patients was noted as the most significant motivator for providers to introduce clinical trials, followed by their desire to contribute to science.
- In terms of challenges relating to finding time, respondents indicated that identifying clinical trial options in other VA sites was the most challenging action, followed by identifying clinical trials outside of the VA.
- When asked about challenges relating to discussing and managing clinical trial participation, respondents indicated that dealing with the extra work of the referral process for trials outside of the VA system was the most significant challenge.
- With regard to factors that could make clinical trial referral and enrollment easier, respondents rated internal VA nurse navigators as the most helpful option and research coordinators contacting cancer teams as the second most helpful.
Semi-structured interviews revealed the many factors that influence providers' referring behaviour.
Following the survey, semi-structured interviews were conducted with eight VHA providers. These providers included one nurse practitioner, one physician assistant, five staff physicians and one fellow.
The data gleaned from the interviews was evaluated using a thematic analysis approach. The resulting themes were:
1) Structural clinical trial enrollment determinants - Many providers spoke of financial barriers for patients, scarcity of trials within the VHA, and lack of clarity concerning financial coverage of external trials as key barriers to clinical trial enrolment.
2) Provider enrollment determinants - In terms of factors that contribute to whether or not providers introduce clinical trials as options to their patients, time constraints were noted as a key barrier by respondents. On the other hand, contributing to science and improving patients' quality of care were both identified as key motivations for introducing clinical trials to patients.
3) Patient determinants - Providers indicated that mistrust in the medical system, lack of support, comorbidities, and limited education are often factors that prevent patients from enrolling in clinical trials.
The Behavioural Journey Map visually depicts the referring and enrollment decision-making process.
Based on the insights gleaned through the literature review, survey, and interviews, the team developed a behavioural journey map to represent the complexity of the clinical trial referral process through the Behavioral Map (Figure 1). This map presents the identified barriers to clinical trial referral divided into four domains: clinical, physician, systematic, and patient. These barriers are then grouped by stage of the referral process. Finally, the map presents key decision points and possible outcomes (i.e., whether the patient is enrolled or not enrolled in a trial). The LLS team will use this map to support the VHA in implementing tools to encourage clinical trial referrals at the appropriate stage in the consideration, referral, and enrollment process. The map also serves to highlight challenge points as well as key barriers that should be addressed.
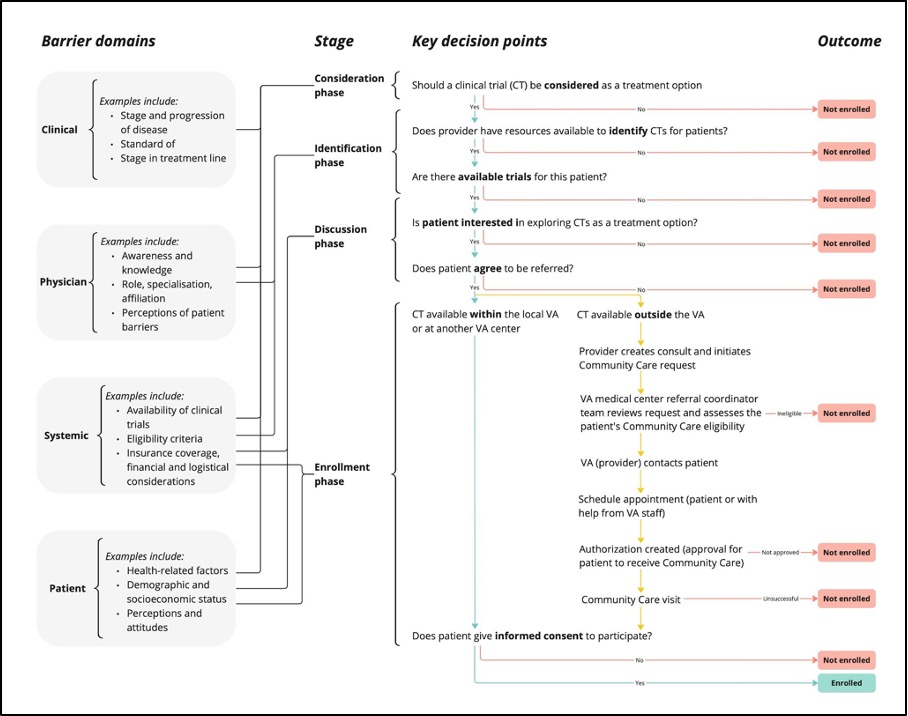
Referring patients to clinical trials is a complex, multi-directional process.
This project not only revealed that the process of deciding to refer patients to clinical trials is a contextually-dependent and, at times, non-linear decision making process, it also yielded critical insights about what factors influence VHA providers' decision to refer patients to cancer care clinical trials. For example, lack of time emerged as a key barrier to clinicians discussing trials with their patients, a finding that was consistent across the literature review, survey, and interviews.
In addition, our research indicates that providers within VHA healthcare system may face unique challenges when considering clinical trials as an option for their patients, such as a dearth of information about clinical trials in other VHA sites and outside of the VHA as well as lack of clarity regarding how to refer patients to community-care trials. In addition, VHA oncology providers serve a patient population that often faces challenges such as transportation needs and lack of support, which can impede patients from trial participation. While many of these barriers can also be seen in the general patient population, these challenges appear to be heightened among veteran patients, a population that often has distinct characters and needs.
Recognising the specific characteristics of VHA patients and the particular challenges that VHA providers may face is critical to bolstering clinical trial participation. Continuing to implement supportive mechanisms and tools, such as Clinical Trial Nurse Navigators, will be essential for increasing oncology clinical trial referrals and enrollment within the VHA.
You can access the full paper here.